Professor Kazem Fathie, M.D., F.A.C.S., F.I.C.S.,Ph.D.
Abstract
This report documents the experience of one neurosurgeon performing cervical fusion using a technique that avoids iliac bone grafts and provides immediate stabilization of the spine. More than 200 patients underwent anterior cervical diskeetomy and methyl methacrylate fusion. No increased neurologic deficit, wound infection, cerebrospinal fluid fis- tula, direct damage to the esophagus or trachea, or hemorrhage requiring transfusion occurred. None of the patients required reoperation at the same level. The overall results compared favorably to reported series with bone grafts or bankbone.
SINCE THE DISCOVERY of methyl methaerylate (1), the plastic material has been used in a variety of orthopedic and neurosurgical procedures (2). Anterior cervical fusion as described by Robinson and Smith (3) and Cloward (4) required an iliac bone graft. As early as 1955, Cleveland (5) described the use of methaerylate for spinal stabilization after disk surgery. Other authors (6-12) had reported acrylic fusion, but Rask (13) reviewed over 1600 methyl methaerylate anterior cervical fusions and credited Cantu (14) and Cruickshank (15). This paper reports the author’s experience with a cervical fusion technique that avoids iliac bone grafts and provides immediate stabilization of the spine.
Methods
Cloward’s (4) instruments were employed to expose the appropriate disk space, to remove the nucleus pulposus and any spondylotic spurs, and to spread the vertebral bodies. A lodging for the cement was created using a power drill in the midportion of the upper and lower vertebral bodies (Fig.1). This dumbbell shape prevented the methyl methacrylate from slipping backward toward the spinalcord or forward toward the anterior spinal ligament. Prior to mixing and pouring, the posterior-aspect of the disk space is coated with Gelfoam to prevent leakage of the plastic into the epidural space. As the semiliquid plastic material is delivered to the interspace with a 10 cc syringe and a flexible no. 14 intercath, the vertebral body distracter is removed. The methyl methaerylate is copiously irrigated with saline as the heat of fusion takes place. Closure of the muscle, fascia, and skin is performed as described by Cloward (4).
The hospital stay is only one or two days, and no collar is necessary in the immediate postoperative period. The patient may resume normal activity within weeks from the date of surgery.
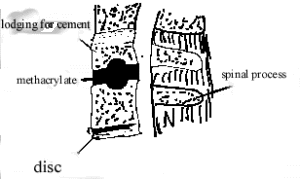
Fig. 1 Artists drawing of acrylic fusion
Results
More than 200 patients underwent anterior cervical diskectomy and methyl methaerylate fusion in this series. No patients had complications of increased neurologic deficit, foreign body reaction, wound infection, cerebrospinal fluid fistula, direct damage to the esophagus or trachea, or hemorrhage requiring transfusion. None of the patients required reoperation at the same level.
Discussion
In 1975, Hankinson and Wilson (16) reported the results for a series of anterior cervical diskectomies performed with the operating microscope but without fusion. The results without a bone graft from the ilium were comparable to those of Cloward (1) and Robinson and Smith (2). Never- theless, the potential for increased foraminal stenosis and instability exists. Eliminating complications associated with obtaining a graft from the iliac crest or with maintaining the bone in situ is desirable. The methyl methaerylate technique allows for preservation of the normal disk spacing and avoids the foreign body reaction reported with some bank bone. The fact that no collar is needed during the period of fusion meets with high patient approval.
Summary
The addition of methyl methaerylate fusion to standard anterior cervical diskectomy for a herniated cervical disk offers a number of advantages. Other than a small number of Cloward instruments, only a power drill and the cement are needed; normal disk spacing is maintained; no bone graft is performed; stabilization of the spine is immediate; and no collar is required. Early return to normal activity is possible following this procedure.
References
1. Henrichsen E, Jansen K, Krogh-Poulsen W. Experimental investigation of the tissue reaction to acrylic plastics. Acta Orthop Scand 1952; 22:141-146.
2. Glaser HT. The local effect upon bone, cartilage and joint tissue of the polymerization of methyl methaerylate in situ. Surgical Forum, Am Col Surg 1958; 8:550-554.
3. Robinson RA, Smith GW. Anterolateral cervical disc removal and interbody fusion for cervical disc syndrome. Bull Johns Hopkins Hosp 1955; 96:223-224.
4. Cloward RB. The anterior approach for removal of ruptured cervical discs. J Neurosurg 1958; 15:602-617.
5. Cleveland DA. The use of methyl methaerylate for spinal stabilization after disk operations. Marquette Med Rev 1955; 20:60-.64.
6. Hamby WB, Glaser HT. Replacement of spinal intervertebral discs with locally-polymerizing methyl methacrylate. Experimental study of effects upon tissues and report of a small clinical series. J Neurosurg 1959; 16: 311-313.
7. Cross GO, White HL, White LP. Acrylic prosthesis of the fifth cervical vertebra in multiple myeloma. J Neuro- surg 1971; 35:64-67.
8. Hoppenstein R. Immediate spinal stabilization using an acrylic prosthesis (preliminary report). Bull Hosp Jt Dis 1972; 72:66-75.
9. Hansebout RR, Bloomquist G. Acrylic spinal fusion. J Neurosurg 1980; 53:606-612.
10. Clark CR, Keggi KJ. Stabilization of the cervical spine using methyl methacrylate. A long-term clinical follow-up. Orthop Trans 1980; 4-41-42.
11. Harrington KD. The use of methyl methacrylate for vertebral body replacement and anterior stabilization of pathological fracture-dislocation of the spine due to metastatic malignant disease. J Bone Joint Surg 1981; 63A:36-46.
12. Bryan W, Inglis AE, Sculco TP, Ranawat OS. Methyl methacrylate stabilization for enhancement of posterior cervical irthrodesis in rheumatoid arthritis. J Bone AA:M-18. Joint Surg 1982; 6
13. Rask MR. “Original” Cruickshank anterior cervical fusion (ACF). Report of 84 patients. J Neurol Orthop Med Surg 1992; 13:11-20.
14. Cantu RC. Anterior spinal fusion using methyl methacrylate (acrylic). Int Surg 1974; 59:62-65.
15. Cruickshank JW. Routine use of methyl methacrylate (MMC) in disks. J Neurol Orthop Med Surg 1983; 4:17- 18.
16. Hankinson HI, Wilson CB. Use of the operating microscope in anterior cervical diseectomy without fusion. J Neurosurg 1975; 43:452-456.
