KAZEM FATHIE, M.D., F.A.C.S., F.I.C.S., Ph.D.
THE patient whose case I shall describe had a large aneurysmal tumor of the internal carotid artery. It had ruptured, and the patient had been treated previously for acrornegaly. I am reporting it because of the very interesting nature of the disease, and also because I want to point out the advisability of arteriography in cases of acromegaly, and especially in ones associated with unilateral third-nerve palsy.
CASE REPORT
A 53-year-old white female was first seen in 1955 at Grady Memorial Hospital, Atlanta, Georgia, because of a long history of renal calculi, with slightly elevated serum calcium and 24-hour calcium excretion, a normal phosphorus and a non-toxic nodular left thyroid gland. She underwent a left hemithyroidectomy on October 24, 1955, and an exploration for parathyroid adenoma was negative. An intravenous pyelograrn demonstrated a stone in the region of the right kidney, and suggested the presence of a stone on the left. An endocrinologic study in July, 1958, revealed an elevation in calcium and a decrease in P04. X-rays of the skull at that time showed the sella turcica in the upper limits of normal, and a squaring of the head and metacarpals suggesting acrormegaly. They measured 13 to 14 mm. in AP diameter, and 6 to 7 mm. in depth. The patient then noticed enlargements of her head, face, hands and feet, and she was unable to wear her wedding ring at all by August 7, 1958. She was followed in the general clinic until April 10, 1961, but repeated skull x-rays showed no changes in the pituitary fossa. At the same time she complained of blurring of vision in the left eye, and diplopia. When she removed her glasses, she developed ptosis of the left upper eyelid within a short time, and upon awakening from deep sleep, she had dilation of the left pupil accompanied by pain in the left eye. Her visual fields were normal. She came to the Emergency Room twice complaining of pain behind the left eye, and on April 24, 1961, she was given a complete work- up. Her blood pressure was 185/110 mm. Hg, her pulse rate was 72/min., her respirations were 18/min., increases were noticed in the sizes of her hands and feet, and she was admitted for tests to rule out acromegaly. On her admission, May 8, 1961, repeated visual- field tests were normal, and the significant laboratory work included a P04 of 3.4 mg. per cent, a calcium of 10.1 mg. per cent, a creatinine of 44 (urine), a repeat calcium of 12 mg. per cent, and a cerebrospinal fluid protein of 41 mg. per cent and a normal opening pressure. On May 27, 1961, pneumoencephalography was performed, and the findings were consistent with a pituitary mass and clinical acromegaly. A V.D.R.L. was negative, and the cerebrospinal fluid was normal. Endocrinologic and neurologic work-ups again supported acromegaly and possible adenorna of the pituitary gland. Eye and visual-field examinnations were again normal. On June 9, 1961, she was discharged with a left third-nerve paralysis but a normal electrocardiogram. She was followed in Endocrine Clinic. The patient had noticed an increase in the size of her hands and feet for the first time in 1930, after the birth of her first child. At that time her shoe size increased from 8 to 10. There were no menstrual irregularities. For the first time, on February 11, 1963, the patient was seen by the Department of Neurosurgery, and a neurologic examination revealed paralyses of the left third, fourth, fifth, sixth, seventh and twelfth nerves, plus ipsilateral hemiparesis and a history of headache. She suddenly became unconscious and unresponsive. A tracheostomy was performed, and neurologically she had a slight stiffness of the neck. Her reflexes were exaggerated, and she had a Babinski sign bilaterally. The left pupil remained dilated, but the fundus was normal. A lumbar puncture revealed normal findings. The opening pressure and the color were within normal limits. It was felt that the patient had bled into the adenomatous tumor, but that bleeding couldn’t account for all of her symptoms. So she was observed until February 18, 1963, and then bilateral carotid and bilateral vertebral arteriograms were performed.
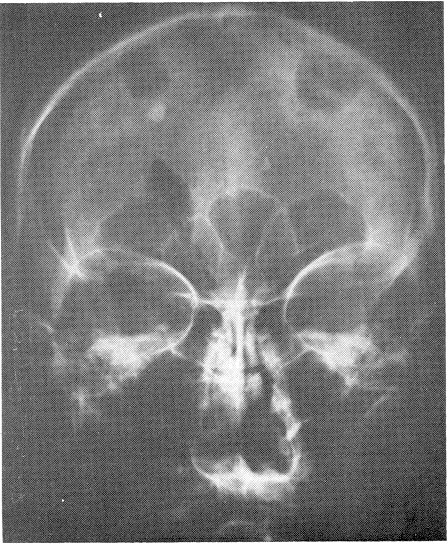
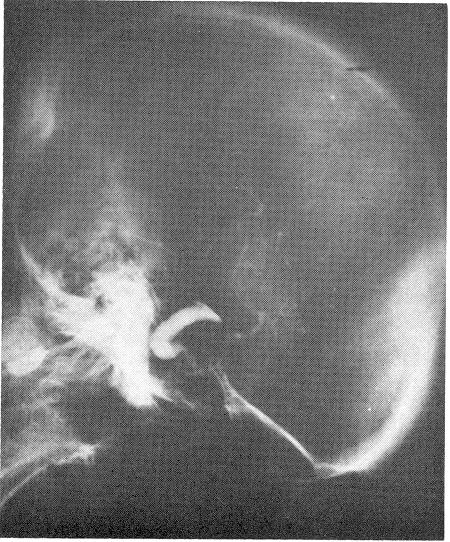
The vertebral arteriogram was completely normal, but the left carotid arteriograrn at that time revealed marked spasm and narrowing of the internal arteries just proximal to the cavernous portion. At the level of the posterior communicating arteries, an unusually long saccular vessel was shown to be present. There seemed to be a small aneurysm at the proximal end of that sac, poor filling of the left middle cerebral beyond the level of bifurcation, and no filling of the left anterior cerebral. The large saccular vessel extended posteriorly and towards the temporal lobe. The right carotid arteriogram revealed excellent filling of the middle cerebral artery and both anterior cerebral arteries. The anterior cerebral vessels were displaced toward the right side by about 1.5 cm. The patient was taken to the operating room the next day, and ventriculography was done. This revealed a marked displacement of the right lateral ventricle and its temporal horn to the right side. In addition, there was a marked displacement of the third ventricle. The nonlocalizing character of the displacement was consistent with the presence of diffuse subdural bleeding, as well as probable local hemorrhage into the temporal horn. A large left frontoparietal temporal craniotomy was performed. The dura was under pressure and bulging. A small incision was made over the dura, and subdural clots (organized, with no membrane) were proved. Gradually, a massive amount of clotted blood was removed, and the temporal lobe and silvan fissure were pushed up by the basal clot. A large, pulsating tumor was seen, with a plug of clot sitting in the ruptured area of the aneurysmal sac. At that point, the operation was stopped, and exposure of the common carotid artery, as well as the internal and external carotid arteries in the neck on both sides, was done. We noted that pressure over the common carotid artery and occlusion on the left side stopped the pulsations of the carotid artery intracranially, and pulsations of the intracranial sac. The sac shrank slightly, but when pressure was removed it pulsated again and returned to its former size. It extended posteriorly to the mid portion of the sella turcica, and anteriorly to the cavernous sinus. Because of its huge size, a wrapping of muscle and Gelfoam was applied to it, and the clots were cleaned from its base. The craniotomy was then closed, a Crutchfield clamp was applied to the left internal carotid artery in the neck, and the patient was transferred to the recovery room. She gradually woke up, spoke, and tolerated the complete ligation of the clamp without incurring hemiparesis, hemiplegia
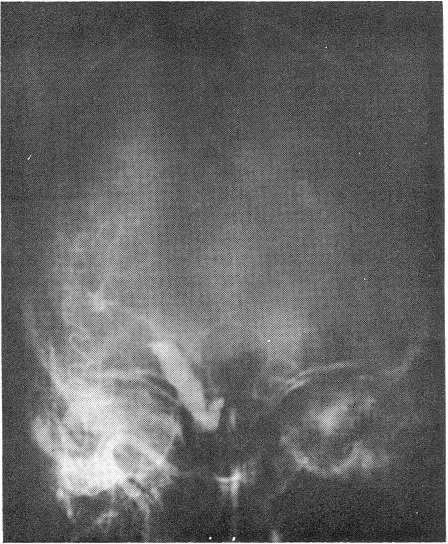
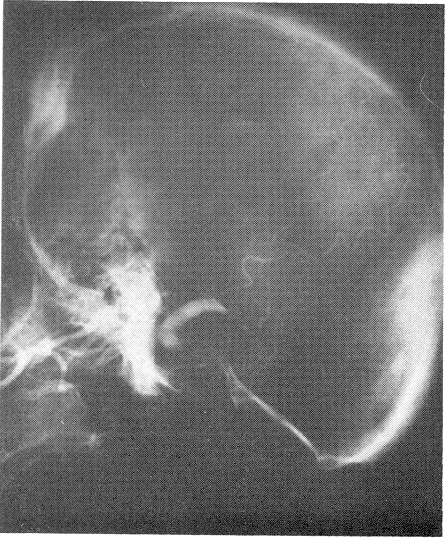
or aphasia. Her state of consciousness returned to the completely normal. lpsilateral hemiparesis cleared within a week, and gradually cranial nerve XII, then VII and then VI were cleared. The patient became ambulatory, and was discharged on May 2, 1963, with palsy only of the third left and possibly the fourth left nerves.
DISCUSSION
Although many authors such as J. C. White and W. A. Hamby have reported previously on large intrasellar aneurysms simulating hypophyseal tumors, very few have emphasized their associa- tion with acromegaly. In the case I have reviewed, it is noteworthy that after all of the diagnostic procedures for acromegaly it remained for arteriography to reveal a further problem-an aneurysrnal tumor or large aneurysmal sac. I feel that it is superfluous to recount all of the articles that have been written on this subject. From a study of the case presented above, and from a perusal of a few references, the reader can familiarize himself with this type of aneurysmal tumor.
SUMMARY
The purpose of this paper has been to point out the problem of diagnosis in cases of large aneurysms, and to emphasize the necessity of arteri- ography in cases of acromegaly and cases of suspected intrasellar mass-especially when there is an associated third nerve palsy or ophthalmoplegia.